Around 500,000 people throughout the UK have been diagnosed with IBD – an umbrella term for one of several bowel conditions.
But what happens to your body if you have ulcerative colitis or Crohn’s disease?
We take a look at some of the most commonly-asked questions about the illness, looking at the symptoms, treatments and potential next steps.
What is IBD?
Inflammatory bowel disease (IBD) is an umbrella term, mainly used to describe ulcerative colitis and Crohn’s disease.
Both are lifelong conditions where the body’s immune system begins attacking itself, often causing swelling and sores in your gut.
Ulcerative colitis only affects the person’s colon, or large intestine, while Crohn’s can have an impact on any part of the digestive system.
These ulcers can bleed or create mucus, which weakens the body’s ability to digest food and process nutrients.

IBD can have similar symptoms to irritable bowel syndrome (IBS) which does not cause inflammation or blood loss.
Around 500,000 people across the UK have been diagnosed with either Crohn’s or colitis.
What are the signs of IBD?
The symptoms of IBD can differ from person to person, but generally involve:
- Stomach cramps or pain
- Recurring diarrhoea, which may contain blood
- Weight loss
- Extreme tiredness
Sufferers can often switch between flare-ups and periods of remission, with the severity of symptoms varying between patients.
Is IBD treatable?
It’s not known exactly what causes IBD and there’s currently no cure – but there are medications available to ease symptoms.
If someone has ongoing issues, however they may need surgery to repair damage or remove part of their bowel.

The NHS estimates around 20% of ulcerative colitis patients have severe symptoms that do not improve with medication, while 60-75% of Crohn’s patients may require an operation.
As better treatments become available, the risk of someone with IBD requiring surgery is lowering all the time.
What would surgery involve?
An operation could be needed if inflammation has caused scarring and a narrowing of the intestines, if medication fails, or if an abscess has formed.
Sometimes the section connecting the large and small bowel has to be removed, and the rest is joined back together.
For some, however, surgeons need to remove all or most of the colon.
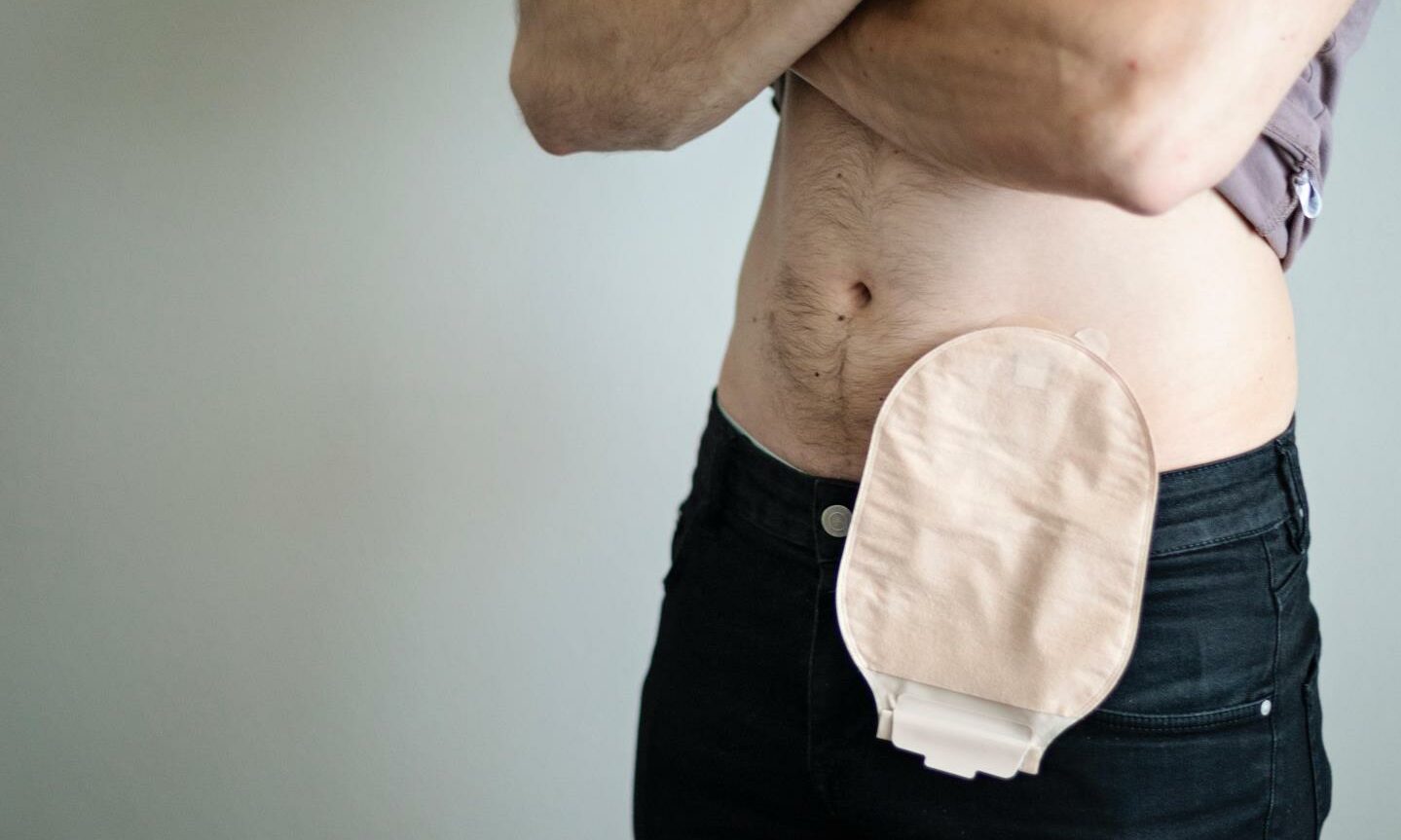
Depending on the surgery carried out, the intestines could then either be attached to the rectum, or a stoma – an opening on the abdomen – created, with a bag fitted to collect waste.
Should I go to my doctor?
If you’re concerned about your health, you should book an appointment with your GP to discuss your symptoms.
Charity Crohn’s & Colitis UK has created a guide for chatting to your doctor, and recommends noting potential symptom triggers ahead of time.
Physical examinations, blood tests and checking your stool can help rule out certain health conditions, and you may be referred to a specialist gastroenterology team for an endoscopy to look at your gut in more detail.
I have an IBD diagnosis – what next?
The charity also runs a wide support network with more than 46,000 members, spread out across 50 local chapters.
It also provides information on its website, and its helpline on 0300 222 5700.
April Trawicki, support services manager at charity Crohn’s & Colitis UK, said: “Hearing you have Crohn’s or Colitis (the two main forms of Inflammatory Bowel Disease – IBD) can be overwhelming, but there’s lots of support out there.
“Our website is full of support and resources, we’ve got a practical to-do list to guide you through diagnosis, a wealth of information about life with Crohn’s or Colitis, and blog posts on any topics you might have questions about.”