It is the ‘cradle to grave’ health service which was created to provide free and universal access to healthcare, and has helped shape the experiences of birth, life and death for the majority of the British public since 1948.
But as the 70th anniversary of the National Health Service (NHS) approaches on July 5, how true does it remain to those founding principles, and what can be done to improve its fortunes in future?
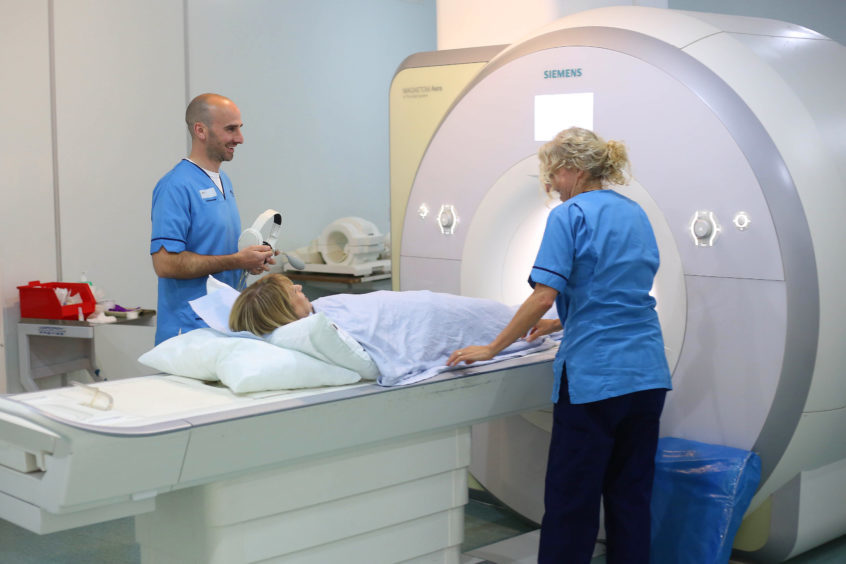
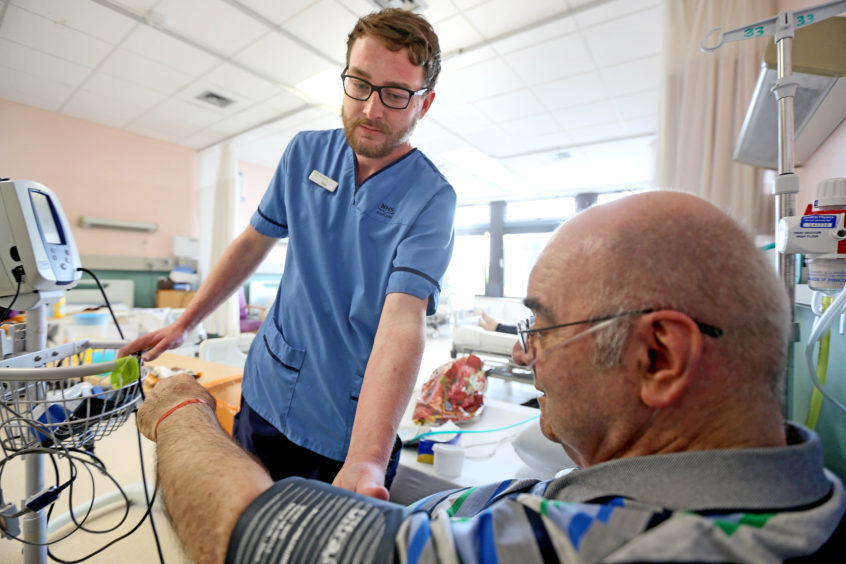
In the first of a four-part mini-series looking at the achievements and challenges facing the NHS, we speak to some of those working at the coalface in Tayside and Fife to find out what it’s like working on the frontlines and to hear what the potential solutions are to the challenges ahead.
Over the next few days, we’ll hear how the NHS has dramatically helped raise life expectancy and expectations.
However, it has also become a “victim of its own success” as the pressures of an ageing population mount, treatments and technologies become more expensive and budgets become tighter.
We hear different opinions on funding, management and how to deal with staff recruitment/retention pressures.
However, we also hear how the NHS continues being at the forefront of global research and development with Dundee-based researchers amongst those working on projects that could save lives around the world.
According to the most recent report into the state of the NHS in Scotland, published in October 2017, the nation’s health is not improving and a failure to put key measures in place is threatening future care provision.
The annual review carried out by Audit Scotland concluded that Scotland’s NHS, which is devolved to the Scottish Government, is struggling to keep up with the challenges of an unhealthy population, tighter budgets, staff recruitment problems, more expensive medicine and a “demanding public and political environment”.
The report said that more people are waiting longer to be seen, the majority of national performance targets were not met and general practice is under pressure from ongoing recruitment problems and low morale.
The Auditor General noted that, despite this, staff are committed and overall patient satisfaction is high.
However, costs are increasing and there is a growing demand for services.
Although the health budget was £12.9 billion in 2016/17 – 43% of the Scottish Government budget, up from 38% in 2008 – unprecedented levels of savings of almost £390 million had to be made in order to break even.
The report said there are some signs of progress in areas such as integrating health and social care, developing better data and embedding a “realistic medicine” approach.
However, it added that key building blocks still need to be put in place by the Scottish Government, NHS boards and integration authorities.
These include a long-term framework clarifying how moving care into the community will be funded, along with greater flexibility for NHS boards on financial planning.
Other recommendations include creating a comprehensive approach to workforce planning, including a cost breakdown.
The man leading on the development of an integrated clinical strategy for NHS Tayside says it is “inevitable” that there will be controversies when a series of proposals for changing healthcare in Tayside are shared with the public over the summer.
Professor Colin Fleming, who is a consultant in dermatology at Ninewells Hospital and the lead in NHS Tayside’s Clinical Alliance, said the Transforming Tayside agenda aimed to develop new service models in response to the “significant challenges” facing the NHS caused by an ageing population, growing demand for services, workforce challenges and continuing pressures on public finances.
In an interview with the Courier at Ninewells as work continues behind the scenes on a series of “ghost proposals” that will be shared with the public within months, Professor Fleming said: “By the middle of July we need to have set up a series of possible options for how we change healthcare in NHS Tayside. Those options need to be fully costed and narrowed down to fewer options.
“There’s then a five-month consultation which is really about ‘what is the public view of this and what is the political acceptability of the changes we are suggesting?’
“There will be a series of proposals about how we change healthcare delivery in Tayside, and those proposals need to go out for public consultation before reporting back to the board by December.
“One example we’ll need to consider very carefully is a new elective care centre for delivery of surgery – but where we put that in NHS Tayside has yet to be determined and that has to go through a process where you carefully look at the clinical and financial considerations.”
Professor Fleming said that fundamentally, NHS Tayside was trying to pull together a plan which “starts with looking at what we really need.”
And at the heart of that discussion, he said, was the way in which acute hospital services are delivered.
“We want to think of that as the starting point – how do we best deliver those services?” he said.
“How do we re-arrange our beds to best deliver those services? How do we maximise the way our theatres are run to look at those services?
“Because if you get that bit right – that flow of emergency stuff coming through – then that lets you know what you can do in a more planned fashion.
“The next bit of the planned fashion is thinking about how we deliver planned care in a cleverer way.
“For example we know with surgical techniques, modern anaesthetics, we can change many of those patients from being inpatients in hospital to being day patients spending more time at home. One of the core planks of what we would like to do is really maximise the day case patient opportunities.
“That does two things – it gives you better outcomes because patients are not hanging around in hospital beds.
“But it also reduces the cost of surgery because you are not paying for those patients to stay in a bed overnight. You don’t have the nursing staff and all the associated costs with that.
“That’s an example of how we think we can really get efficiencies in the service and actually improve the care of patients.”
Professor Fleming said there was “no single answer” to the pressures facing the NHS. Some fundamental questions had to be asked by society about what’s a “fair expectation” of health services.
His biggest concern was the global scale of the health care challenge and the need to successfully bring the public along as proposals for review emerged.
Simply “throwing money” at the system, however, was not the answer.
He added: “If you look at the USA – they spend more than twice the budget we do per person on healthcare and they have the same outcomes as Costa Rica that spends one eighth of what the USA spend.
“Throwing money at healthcare in an un-thought of manner does not lead to good outcomes and this is something where I think we are learning and it’s one of the reasons I think we can be optimistic about improving NHS Tayside.
“We have a lot of doctors who are beginning to learn about finance and a lot of doctor managers who are learning how to manage better. We have a lot of individuals now working in joined up ways to understand the whole system. And we haven’t had to do that actually until relatively recently.
“The problem with being around for 70 years is that it has aggressed 70 years of good practice and 70 years of bad practice in the culture.”
Essex-born Cambridge University graduate Dr Margaret Hannah, 56, has been Fife’s consultant in public health since 1996.
Her decision to study medicine was influenced by her mother’s experiences of working as a nurse during the early years of antibiotics, and her civil servant father undergoing a pioneering and ultimately lifesaving fibre optic brain tumour operation on the NHS in the mid-1970s.
But those early technological breakthroughs almost pale into insignificance compared with some of the developments she has experienced as a health care professional since.
The development of fibre optic knee surgery; the development of IVF for infertile couples in the 1980s; life-saving developments in transplant surgery and the ability to save the lives of low birth weight babies are just some examples that have transformed lives.
Wider post-war public health improvements including the vaccination of children, better nutrition and housing conditions, cleaner air and water, the expansion of literacy and education and the development of workplace Health and Safety, mean the UK population has generally been living longer and healthier than ever before.
Yet the rapid progress seen over the last 70 years has come at a price with lifestyle diseases such as cancers and diabetes on the rise, the demands of an ageing population taking their toll on resources and the amazing drugs and technologies available becoming increasingly expensive.
It’s meant that health professionals have had to find and continue to search for increasingly innovative solutions with some potentially difficult decisions about the delivery of care yet to be made.
There’s an ongoing re-think, for example, of how the rising number of older people can have their stays reduced in acute hospitals and a greater realisation that patients benefit from immobilising in the comfortable surroundings of home during the last decades of life.
Realistic Medicine, launched by Scotland’s Chief Medical Officer, is shifting health professionals’ focus from “doing more to doing things better and more effectively.”
It’s now recognised, for example, that putting patients on more than five medications at one time is likely to have a detrimental impact on health. “Shared decision making” between doctors and patients about the potential benefits or hazards of a treatment will become more common place.
But Dr Hannah says it’s very important to understand that the NHS is only one part of how the population’s health is maintained. The pressures of an ageing population are being felt throughout the western world and many of the issues are trans-sectoral.
“What we are faced with now is a changed pattern of disease – it’s just a case of the NHS not moving fast enough to adapt to that,” she said.

“This is the century of biotechnology – we haven’t seen the half of it yet, But it shouldn’t ever be forgotten that the NHS is fundamentally a human system with patients at the heart. That should never be lost sight of as the NHS moves forward.”
According to retired NHS Fife chief executive John Wilson, a “responsible, national, conversation” about the type of NHS we want, what it will and will not provide and an assessment of how much resources are needed to achieve this should take place as a matter of priority.
The 60-year-old, who worked in the NHS for 35 years before retiring in 2014, said this process needed to emphasize the personal responsibility everyone has for their own health and that of their children.
Reductions in smoking, encouraged by smoking bans in public places have contributed to a reduction in heart disease and stroke.
Action on alcohol consumption should have similar impacts on alcohol related ill health while tackling obesity will also have a profound impact.
However, while Mr Wilson believes devolution has brought great benefits to the NHS in Scotland through accountability and its ability to target specific problem areas, he has called on politicians to stop using the health service as a “political football”.
He said there needs to be cross party understanding of the problems faced by the NHS in the 21 Century and recognition that whatever party is in power at whatever tier of government, the problems need to be faced up to and consensus reached on how to resolve them.
It’s also important, he said, that the NHS is not looked at in isolation because poverty, unemployment, and poor housing all have an impact.
“I think it’s inevitable that the NHS is political because it is a public service and we use public money and we are directed by the Scottish Government,” he said.
“But what I think is worrying is the fact that the NHS is used as a tool to beat the government up. That is demoralising for those that work in the service and it must be concerning for the patients thinking that the service isn’t being properly managed.”
Mr Wilson said there would be a “lot of opposition” if attempts were ever made to privatize the NHS. He said it was a “huge achievement” that the service still exists and retains its founding principles after 70 years.
However, he believes the biggest threat to its future is the “bottomless pit of resources you could put into it.”

In order to solve the crucial problem of delayed discharges there needs to be a clear understanding of the total need for all aspects of health and social care, clarity on the options and alternative models available, accurate assessment of the staffing needs to deliver them and a realistic budget to fund them.
Last week experts in England said taxes are going to have to rise to pay for the NHS if the UK is to avoid “a decade of misery” in which the old, sick and vulnerable are let down.
The Institute for Fiscal Studies and Health Foundation said the NHS would need an extra 4% a year – or £2,000 per UK household – for the next 15 years.
The announcement came days after leading doctors in Scotland wrote to the prime minister calling for more details about the future funding of the NHS.

The presidents of three royal medical colleges north of the border signed a letter to Theresa May regarding her promise, made in March, to bring forward a longer-term plan for financing the health service.
In Scotland, it’s Holyrood that decides what resources are to be devoted to the NHS, in the context of devolved public expenditure.
Of approximately £34.7 billion controlled by the Scottish Government, around £11.9 billion is spent on health.
But is funding the answer to the NHS’ ills?
Professor Dilip Nathwani, the Ninewells Hospital-based director of the Tayside Academic Health Sciences Partnership, prefers Scotland’s funding model to England.
He believes more efficiencies are required and also thinks the NHS needs a “greater slice of overall funding”.
But he also thinks there needs to be a “mature and transparent conversation about how the NHS looks at external funding and commercial opportunities.”
He said: “It is not about the privatisation of health care – I have never bought into that – but if you look at health care systems elsewhere, the way they conduct some business with commercial partners to the gain of the healthcare system needs to be better explored.

“How we can get access to some of the newer technologies, newer drugs? I think those conversations need to be at a different level because I think we can gain from that. It used to be a closed shop that we will have nothing to do with commercial partners.
“At the end of the day it’s the commercial partners that are investing in a lot of innovation and bringing new stuff to us.
“But we need to work with them. We need to tell commercial partners what is the new stuff we want and then adopt that into the new system we require.