Dundee-raised eye surgeon and St Andrews University clinical academic Dr Andrew Blaikie tells Michael Alexander how a pioneering device could save the sight of millions in the developing world.
Despite the progress made in surgical techniques in many countries during the last 10 years, cataract (47.9%) remains the leading cause of visual impairment in all areas of the world, except for developed countries, according to figures from the World Health Organisation (WHO)
In the least-developed countries, and in particular Sub-Saharan Africa, the main causes of avoidable blindness are primarily, cataract (50%), glaucoma (15%), corneal opacities (10%), trachoma (6.8%), childhood blindness (5.3%) and onchocerciasis (4%).
But now pioneering Scots researchers – which include a Fife-based surgeon and scientist – have launched a pocket-sized device which could prevent millions of people in poor countries from losing their sight or hearing.
The breakthrough tool, known as the ‘Arclight’, is being trialled in parts of Africa and Asia to screen patients for the onset of blindness-causing eye disorders such as diabetes, cataracts and glaucoma, as well as retinoblastoma – a rare but potentially fatal type of eye cancer which mostly affects children under five, but which can be cured in 95% of cases if identified early.
The device is also being used in Malawi to detect and treat ear conditions which can lead to deafness, and is already being sold to medical schools and GPs in the UK to help diagnose eye and ear diseases after preliminary studies showed that it was more effective that existing machines which cost hundreds of pounds more.
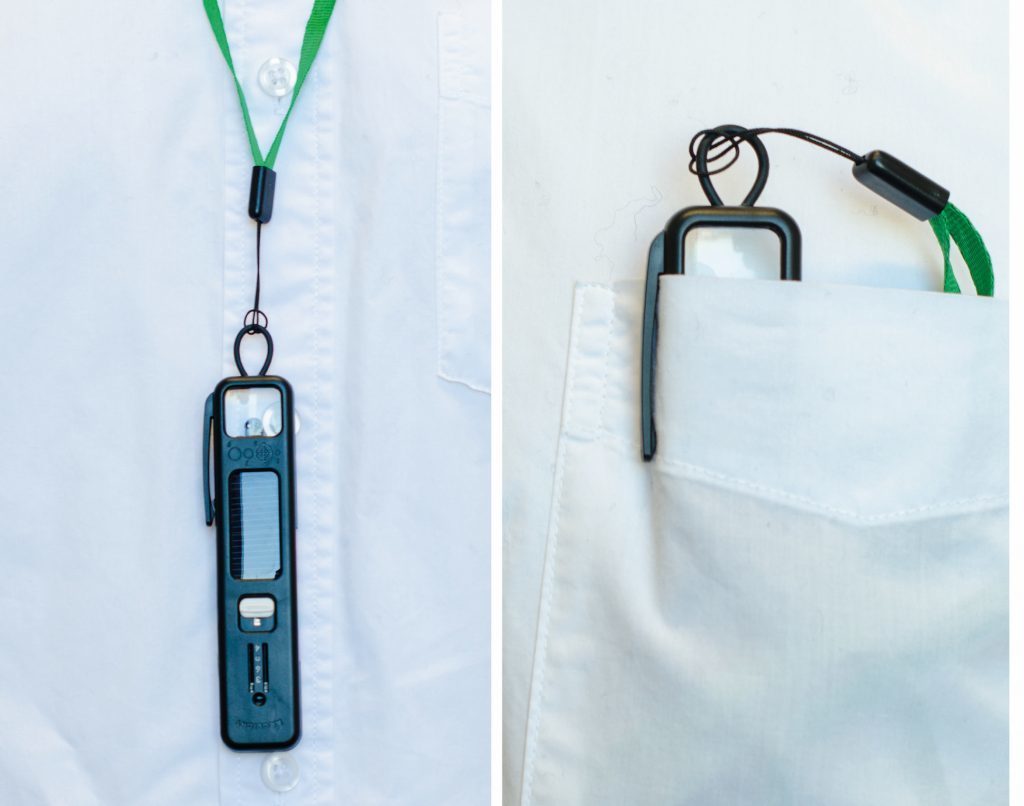
Dr Andrew Blaikie, 47, a clinical academic at St Andrews University, who also works as an eye surgeon with NHS Fife at Queen Margaret Hospital in Dunfermline, said Arclight’s strength was the fact it was pocket-sized, low-cost and solar-powered.
Working with colleagues at Leicester University and University College London, he has been a central member of the team steering the development and testing of the Arclight, which has been designed specifically as an easy-to-use tool for out-reach or screening programs in low-income countries.
It enables users to make instant on-the-spot diagnostic decisions -and a study led from the International Centre for Eye Health in London already shows that it performs as well as traditional devices costing up to 100 times as much.
“Around 285 million people in the world are estimated to be visually impaired, and 360 million hearing impaired, with the majority of cases considered preventable or treatable if diagnosed promptly,” said Dr Blaikie a former pupil of Eastern Primary, Broughty Ferry and Dundee High School.
“Ophthalmoscopes and otoscopes are typically designed for wealthy countries and are complex, heavy, and expensive; their basic designs have remained relatively unchanged for over 100 years.
“Very few practitioners in low and middle income countries have these essential tools.
“If they do, they are typically hand-me-downs that don’t work because they need parts that are hard to find or expensive, such as bulbs and batteries.
“The vast majority of cases of vision and hearing impairment, however, are found in these countries with least access to equipment.
“Using the Arclight an examiner can see the front and back of the eye helping reveal all major blinding conditions such as trachoma, cataract, glaucoma and diabetes. It is ideal for students or any qualified health care worker in low or high resource health care settings.”
A medicine graduate of Edinburgh University, Dr Blaikie gained knowledge of eye problems in the developing world whilst travelling as a student. Later, at Leicester, he was inspired by working with doctors from areas like Sub Saharan Africa who were being trained to treat patients back home.
Dr Blaikie said that through collaboration with the Fred Hollows Foundation and the International Agency for Prevention of Blindness, thousands of units have already been distributed to countries around the world, including Malawi, Ethiopia, Kenya, Tanzania, Rwanda, Ghana, Fiji, Indonesia, and the Solomon Islands, enabling healthcare workers to perform comprehensive eye and ear examinations for the first time.
“The work of the Global Health Team at St Andrews has helped focus attention on the exact needs and challenges of health care workers in low-income countries,” he added.
“We now aim to add internal memory loaded with teaching material and a clip to allow image capture with mobile phone cameras to the next version of the device.
“At the same time we are developing several other potentially disruptive low cost diagnostic tools aimed at serving the needs of health care workers in poorer countries.
“Our studies have also shown the device is an ideal tool for medical students and doctors in the UK too, and through sales here and in other wealthy nations we aim to cross-subsidise distribution to poorer countries such as Malawi where Scotland has strong historical links.”
St Andrews University has now established a spin-off company to promote sales of the device and coordinate the subsidised distribution to low income countries.